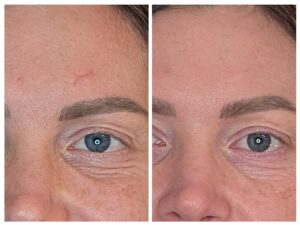
Scars are not simply “damaged skin”—they are the end result of a highly regulated biological repair process. After an injury (whether acne, surgical sutures, or trauma), the skin moves through three overlapping phases:
- Inflammation – immune cells clear debris and bacteria
- Proliferation – fibroblasts deposit collagen and extracellular matrix
- Remodeling – collagen is reorganized over months to years
In normal healing, collagen type III is gradually replaced by stronger, more organized collagen type I. In scars, this remodeling phase is imperfect or dysregulated, leading to visible differences in texture, thickness, or color. (NCBI)
Different scar types reflect different biological errors:
- Atrophic scars (acne scars): collagen loss ? depressions
- Hypertrophic scars: excess collagen, but confined to wound
- Keloids: excessive collagen growth beyond wound boundaries driven by signaling molecules like TGF-? (NCBI)
This matters because treatments work by re-triggering or modifying the remodeling phase—essentially convincing the skin to “heal again, but better.”
When should scars be treated?
There’s a persistent myth that you should “wait until a scar is fully mature.” Evidence suggests the opposite:
- Early intervention (weeks to months) can improve outcomes and prevent worsening (NCBI)
- Treatments like lasers are increasingly used on immature scars to guide collagen remodeling sooner
That said:
- Fresh wounds still need to close first
- Inflammation should be controlled before aggressive procedures
Is it ever too late?
No. Even years-old scars can improve, because collagen is continuously remodeled—just more slowly. However:
- Older scars are more resistant
- Improvement tends to be incremental, not dramatic
Transition: how treatments actually work
Nearly all scar treatments share one principle:
They induce controlled injury to stimulate new collagen remodeling.
The difference lies in how deep, how controlled, and how intense that stimulus is.
Laser Genesis (non-ablative laser): gentle remodeling
What it is:
Laser Genesis uses a 1064 nm Nd:YAG non-ablative laser, delivering heat into the dermis without breaking the skin surface.
Mechanism (scientifically):
- Delivers sub-ablative thermal energy
- Stimulates fibroblasts ? increases collagen production
- Improves microvascular function and mild inflammation
- Promotes gradual dermal remodeling without removing tissue
This aligns with broader laser scar therapy, where photothermal energy stimulates collagen and elastin remodeling in the dermis. (NCBI)
What it’s good for
- Mild acne scarring
- Redness, early scars
- Texture refinement
What it’s not good for
- Deep atrophic scars
- Thick hypertrophic scars
Realistic expectations
- Subtle improvement (often 10–30%)
- Requires multiple sessions (4–8+)
- Minimal downtime ? tradeoff is less dramatic results
A blunt truth: Laser Genesis is often too gentle to significantly remodel established scars, especially compared to fractional lasers.
Microneedling (± PRP/PRF): controlled micro-injury
Mechanism
Microneedling creates thousands of microchannels in the skin:
- Triggers wound healing cascade
- Increases collagen and elastin production
- Improves scar depth and texture (PubMed)
Evidence
- Large study: ?50% improvement in most patients, with many achieving 50–75% improvement (PubMed)
- Systematic reviews confirm consistent improvement in acne scars (PMC)
PRP / PRF addition
- PRP delivers growth factors (PDGF, TGF-?, VEGF)
- May enhance healing and early results
- Evidence is promising but not strong or definitive, especially long-term (PMC)
Realistic expectations
- Requires 3–6+ sessions
- Gradual improvement over months
- Best for:
- Mild–moderate acne scars
- Mixed scar types
Notably, real-world experiences echo this:
“Results build gradually, not overnight… most people need 3–6 sessions.” (Reddit)
Limitations
- Less effective for deep “ice pick” scars
- Results plateau without combination treatments
Chemical peels: surface-level remodeling
Mechanism
- Controlled chemical injury (e.g., glycolic acid, TCA)
- Exfoliates epidermis ± superficial dermis
- Stimulates regeneration and collagen turnover
Best for
- Superficial acne scars
- Pigmentation (post-inflammatory hyperpigmentation)
Realistic expectations
- Mild to moderate improvement
- Requires multiple sessions
- Deeper peels = more results, but more downtime
Limitation
- Cannot significantly improve deep structural scars
Regular facials: supportive, not corrective
Facials:
- Improve hydration, barrier function
- Reduce inflammation
- Support healing environment
But:
- They do not remodel scar tissue meaningfully
Think of them as:
Maintenance—not treatment
Putting it all together: what actually works (realistically)
|
Treatment |
Mechanism depth |
Best for |
Expected improvement |
|
Laser Genesis |
Superficial dermal heating |
Mild scars, redness |
10–30% |
|
Microneedling |
Mid-dermal collagen induction |
Mild–moderate scars |
30–70% (series) |
|
Microneedling + PRP |
Same + growth factors |
Possibly enhanced healing |
Slight boost, uncertain |
|
Chemical peels |
Superficial |
Pigment + shallow scars |
Mild |
|
Facials |
Surface only |
Skin quality |
Minimal for scars |
Key reality check
- No treatment “erases” scars
- Most improvements are incremental and cumulative
- Combination therapy often works best (e.g., microneedling + laser)
Final answers to common questions
How soon should scars be treated?
? As early as safely possible once the skin has healed; early intervention improves outcomes.
Is it too late for old scars?
? No—but expectations must be lower and treatments more aggressive.
Which scars respond best?
- Acne scars ? microneedling, lasers
- Surgical scars ? early laser intervention
- Traumatic scars ? combination approaches
Bottom line
Scar treatment is fundamentally about restarting the remodeling phase of wound healing. The more controlled and deeper the stimulus, the more potential improvement—but also more downtime and risk.
- Laser Genesis: low risk, modest reward
- Microneedling: strong evidence, good middle ground
- PRP/PRF: promising but not definitive
- Peels/facials: supportive, not transformative